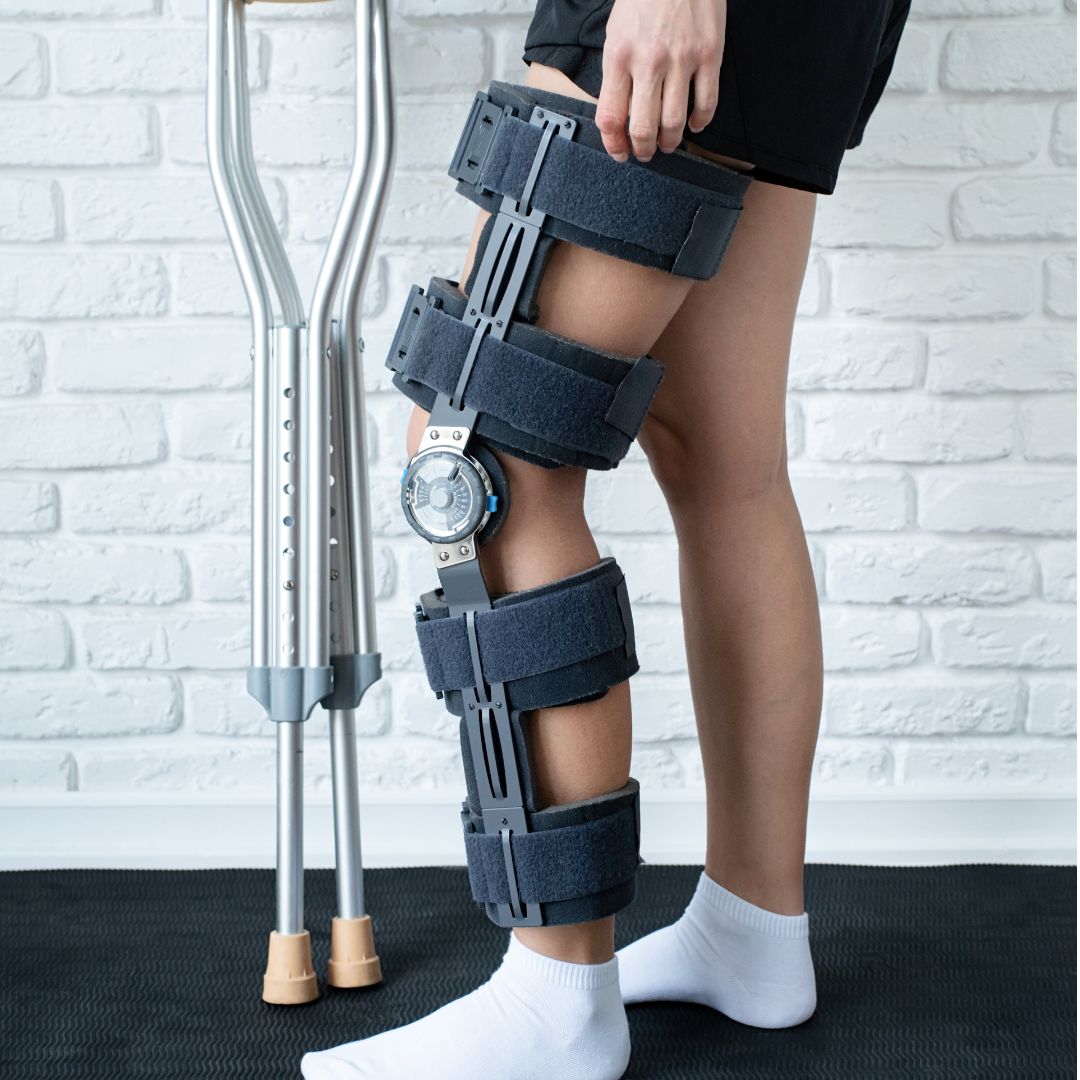
RoboLens FT3D Knee Resurfacing
RoboLens FT3D Knee Resurfacing is a precision-based approach that supports individualized surgical planning and anatomy-specific execution for selected knee arthritis patients.
our specialities
Advanced Precision Orthopaedic Treatments
Robotic knee replacement uses technology-assisted planning to improve alignment, implant positioning and joint balance for patients with severe arthritis, deformity or stiffness.
- Precision Surgical Planning
- Second Opinions Welcome
- Technology-Assisted Precision Orthopaedics
FAQ
Frequently Asked Questions
Common questions about knee replacement, RoboLens FT3D resurfacing, robotic hip replacement and orthopaedic care — answered clearly.
RoboLens FT3D Knee Resurfacing is a precision-based knee treatment approach that supports individualized surgical planning and anatomy-specific execution for selected patients with knee arthritis. Instead of treating every knee with a standard template, FT3D planning evaluates the patient’s joint geometry, alignment and cartilage damage pattern to guide a more personalized procedure. Suitability depends on arthritis stage, bone quality, ligament condition and overall medical evaluation.
Knee replacement is considered when arthritis pain significantly affects walking, climbing stairs, sleep or daily independence — and when conservative treatments such as physiotherapy, medication and injections have not provided adequate relief. The decision is based on X-ray findings, pain severity, functional limitation and overall health. Not every patient with knee pain needs surgery, and the consultation will help determine the right approach for your specific condition.
Most patients begin walking under supervision within 1–2 days of surgery. By 2 weeks, most manage basic daily activities with some assistance. By 6 weeks, stair climbing and independent walking are improving steadily. Functional recovery continues over 3–6 months. Full strength and return to normal activities usually develops over 6–12 months. Consistent physiotherapy is the single most important factor in achieving a good outcome.
Robotic-assisted knee replacement offers more precise alignment planning and implant positioning compared to conventional instruments. For many patients — particularly those with complex anatomy, deformity or unusual alignment — this precision translates to better functional outcomes. However, the surgeon’s experience and judgment remain the most important factors. Robotic technology enhances good surgical decision-making; it does not replace it. Whether robotic or conventional is more appropriate for you will be determined during evaluation.
Total knee replacement replaces the entire knee joint surface — both the femoral and tibial sides. Partial (unicondylar) knee replacement addresses only the damaged compartment — most commonly the inner (medial) side — while leaving healthy cartilage and bone intact. Partial replacement is suitable only for patients with compartment-specific arthritis and intact ligaments. It is not a universally better option; it is a more appropriate option for selected patients. Both procedures have excellent outcomes when the right patient is matched to the right surgery.
Knee osteoarthritis develops due to gradual cartilage wear over time. Contributing factors include age, excess body weight, previous joint injuries, repetitive load on the knee, genetic predisposition and deformity. It cannot always be prevented, but the rate of progression can be slowed through weight management, regular low-impact exercise, physiotherapy and avoiding activities that repeatedly stress the joint. Early evaluation when symptoms begin allows for more conservative management and better long-term outcomes.
Physiotherapy is appropriate when arthritis is in early or moderate stages and the pain is manageable with activity modification, strengthening exercises and lifestyle changes. Surgery becomes the right conversation when conservative treatment over a reasonable period has not provided adequate relief, when X-rays show significant joint damage, and when daily activities like walking, stairs and sleep are meaningfully affected. A consultation with clinical examination and X-ray review will give you a clear answer specific to your condition.
Simultaneous bilateral (both knees together) knee replacement is technically possible and is performed in selected patients. It reduces total hospitalisation time and recovery period compared to two separate surgeries. However, it carries a higher physiological demand during the early recovery phase. Suitability for simultaneous replacement depends on age, cardiac and lung health, blood parameters, body weight and overall medical fitness. Many patients are better served by staged replacement — one knee at a time, 3 to 6 months apart. This decision is made on clinical grounds.
Modern knee implants are designed and tested to last 15–20 years or longer in appropriately selected patients with normal activity levels. Implant longevity depends on several factors including patient age, body weight, activity type, implant quality, surgical alignment and bone quality. Patients who remain active, maintain a healthy weight and follow up regularly with their surgeon can expect excellent long-term outcomes. Revision surgery is available when needed, and Dr Tarandeep Singh Gill has performed 500+ revision and complex cases.
Your first consultation will include a detailed discussion of your symptoms, activity limitations and treatment history. Dr Gill will conduct a clinical examination of the affected joint — assessing range of motion, alignment, ligament stability and muscle strength. Weight-bearing X-rays will be reviewed and explained to you in clear language. You will receive an honest assessment of your diagnosis and all treatment options — including non-surgical options where appropriate. No decision needs to be made on the day. The goal of the consultation is understanding, not commitment.